
Coronavirus Tidbits #113 1/17/21
Quick links
News Diagnostics Drugs Devices Epidemiology/Infection control Tips Politics Feel good du jour Comic relief Perspective/Poem Bits of beauty
Announcements:
First, there is now a Resources Page here for the most commonly asked questions I’m getting.
Happy to continue to answer your questions/concerns as best I can, so don’t be shy about that.
NEW Post on Forbes:
My latest: 12 Most Common Questions About #Covid Mutations And #Vaccines via @forbes https://t.co/Yn1WmMKxZV
— Judy Stone (@DrJudyStone) January 16, 2021
News
Reinfections
immune responses from past infection reduce the risk of catching the virus again by 83% for at least five months.
The data suggest that repeat infections are rare — they occurred in fewer than 1% of about 6,600 participants who had already been ill with COVID-19. But the researchers also found that people who become re-infected can carry high levels of the virus in their nose and throat, even when they do not show symptoms. Such viral loads have been associated with a high risk of transmitting the virus to others, said Hopkins.
https://www.nature.com/articles/d41586-021-00071-6
~ ~ ~
Health care worker shortage
About 3% to 4% of health care personnel who recover from coronavirus infection are expected to become “COVID long-haulers” as they cope with debilitating symptoms 12 to 18 months after the acute stage of the infection clears.
“As COVID-19 surges again, hospitals are facing a shortage of skilled frontline providers who can meet the relentless demands of caring for these patients,”
Will hospitals try to make any accommodations?
https://www.eurekalert.org/pub_releases/2021-01/mgh-hmh011221.php
~ ~ ~
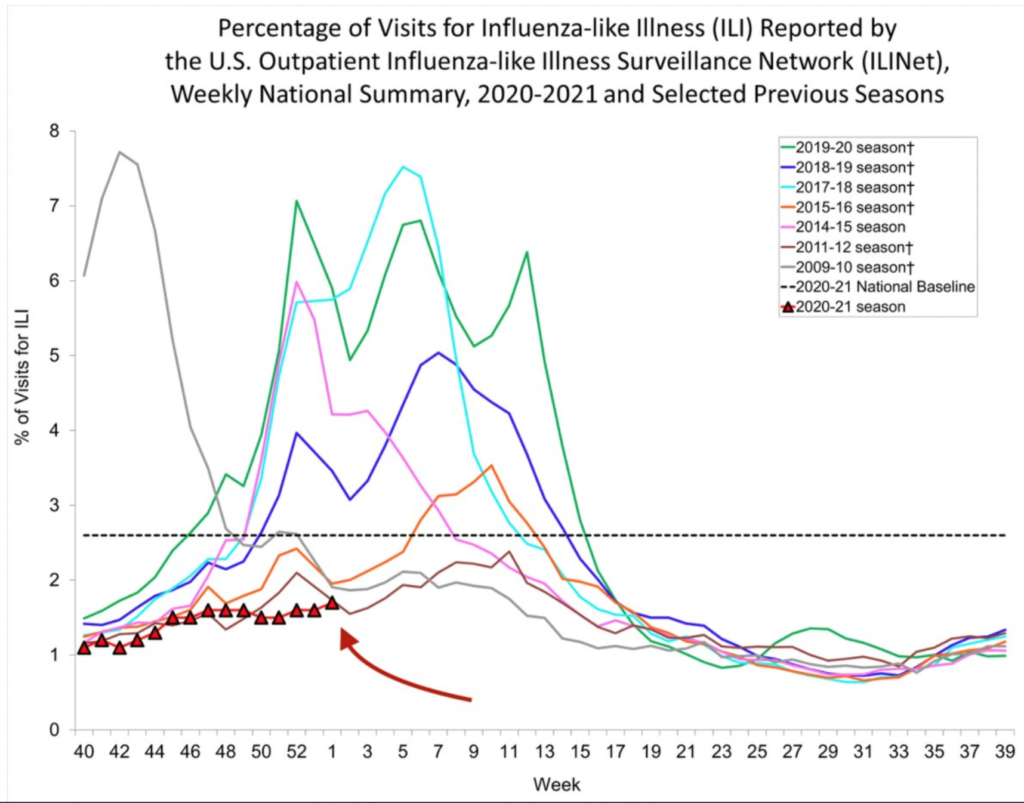
Much less influenza
via @HelenBranswell:
Diagnostics:
still an incredible, negligent lack of rapid, accurate testing.
Drugs:
Although negative, this result is incredibly important and moves forward the treatment of COVID. This was only possible thanks to the generosity of recovered patients and the willingness of current patients to contribute to advancing medical care. We owe you all a great debt.
— Peter Horby (@PeterHorby) January 15, 2021
~ ~ ~
Is the COVID-19 vaccine safe for nursing mothers?
This is a challenging topic because the vaccine trials excluded lactating women. Thus, there are no clinical data regarding the safety of the Pfizer/BioNtech or the Moderna vaccine in nursing mothers. According to the ABM statement, “there is little biological plausibility that the vaccine will cause harm, and antibodies to SARS-CoV-2 [the virus that causes COVID-19] in milk may protect the breastfeeding child.”
Click here to read the ABM statement
https://www.eurekalert.org/pub_releases/2021-01/mali-itc011221.php
~ ~ ~
On hospital leadership: ‘Let’s stop arguing and be pragmatic’ about COVID immunization
“In fairness to hospitals, they should not have been in this predicament where they are a primary site for community vaccinations,” writes Makary, who last week exhorted healthy healthcare workers to sacrifice on COVID immunization for vulnerable neighbors. “Local pharmacies, grocery stores and dialysis centers have extensive experience administering vaccines each year and should have received more vaccine supply.”
~ ~ ~
HHS monoclonal antibody treatment locator
Why are states hiding this information from the public?
In November, the Food and Drug Administration issued emergency use authorization for two monoclonal antibody therapeutics to treat mild or moderate COVID-19 in high-risk, non-hospitalized patients. …States and territorial health departments must opt in to have information for facilities within their jurisdictions available in the locator. The locator launched with 22 state and territorial health departments opting in, and HHS is encouraging all states and territories to participate.
Locator = https://protect-public.hhs.gov/pages/therapeutics-distribution#distribution-locations
~ ~ ~
Disparities:
I'm worried this is happening across the country with communities that are hit hard not the ones getting vaccinated
— Ashish K. Jha, MD, MPH (@ashishkjha) January 17, 2021
Solution is not to slow things down with complex rules
Its to use data to track and proactively target efforts to ensure highest risk folks are not left behind https://t.co/fJK8WK6mPh
~ ~ ~
COVAX is key to both immunizing the world’s poorest people and ending the pandemic.
In a significant moment for the fight against the coronavirus, international funders came together in early June and pooled funding towards an ambitious undertaking: to buy enough COVID vaccines to immunize the 20% of people most vulnerable to the virus worldwide, such as health-care workers and the elderly. High- and middle-income countries would pay into the fund and receive a share of the vaccines procured, and poorer countries would receive vaccines free of charge. But the project, a pioneering effort called COVAX, is struggling to meet expectations.
High-income countries have been buying up large tranches of the current and future vaccine doses directly from vaccine suppliers. Middle-income countries are also negotiating their own supplies. This has left relatively few vaccines for COVAX…
COVAX is competing for these supplies. Some people in the lowest-income countries might need to wait until at least 2022 to get their vaccines.
https://www.nature.com/articles/d41586-021-00044-9
~ ~ ~
COVID’s toll on smell and taste: what scientists do and don’t know
Almost a year later, some still haven’t recovered these senses, and for a proportion of people who have, odours are now warped: unpleasant scents have taken the place of normally delightful ones. Nature surveys the science behind this potentially long-lasting and debilitating phenomenon.
https://www.nature.com/articles/d41586-021-00055-6
~ ~ ~
More vision problems (myopia) in kids
home confinement during the coronavirus pandemic seemed to be linked to a substantial shift toward myopia in students 6 to 8 years old.
Reasons for this, they said, may include less time spent outdoors and more screen time, adding that less outdoor activity is known to be significantly tied to an elevated incidence of myopia in elementary school children.
Devices:
Some of the nation’s most prominent people have begun to double up on masks — a move that researchers say is increasingly being backed up by data https://t.co/MRQ2jHU6j1
— NYT Health (@NYTHealth) January 14, 2021
~ ~ ~
Turn off that camera during virtual meetings–environmental study
May well be true, but ignores the psychosocial benefit of “seeing” other people and reducing the sense of isolation and depression.
Just one hour of videoconferencing or streaming, for example, emits 150-1,000 grams of carbon dioxide (a gallon of gasoline burned from a car emits about 8,887 grams), requires 2-12 liters of water and demands a land area adding up to about the size of an iPad Mini.
But leaving your camera off during a web call can reduce these footprints by 96%. Streaming content in standard definition rather than in high definition while using apps such as Netflix or Hulu also could bring an 86% reduction, the researchers estimated.
https://www.eurekalert.org/
~ ~ ~
Activity trackers
Apple Watch is able to detect “subtle changes in an individual’s heartbeat” up to seven days before the onset of COVID-19 symptoms or a positive test.
study from Stanford, the results of which were released in November, included activity trackers from Garmin, Fitbit, and Apple. The study found that these devices could indicate changes in resting heart rate “up to nine and a half days prior to the onset of symptoms” in coronavirus-positive patients.
The researchers were able to identify nearly two-thirds of COVID-19 cases four to seven days before symptoms, the study says.
“It’s a big deal because it’s alerting people not to go out and meet people,”
https://9to5mac.com/2021/01/16/apple-watch-covid-studies-detection/
Epidemiology/Infection control:
Most SARS-CoV-2 transmission comes from asymptomatic people
A new analytical model suggests that more than half of all SARS-CoV-2 transmission comes from asymptomatic people, CDC researchers reported.
The finding, published in JAMA Network Open, indicates that isolating symptomatic patients with COVID-19 will not be enough to stop the spread of the virus, researchers said.
“These findings underscore the importance of mitigation measures such as wearing masks, social distancing and washing of hands by everyone to slow spread of COVID-19, including from persons without symptoms,”
~ ~ ~
Reinfection?
“Siren” study: antibodies provide an 83% rate of protection against reinfection, likely at least five months.
However, the early evidence also suggests a small number of people with antibodies may still be able to carry and transmit the virus, emphasizing the need to follow coronavirus restrictions
~ ~ ~
More infectious strains require better defenses. Not more of same, better of same.
— Dr. Tom Frieden (@DrTomFrieden) January 16, 2021
Minimize time indoors with others not in your household
Better masks. Surgical, N95, as available. https://t.co/jljpqyznyc
Accelerate vaccination
Treat early
Test, isolate, quarantine
8/
~ ~ ~
Transmission is facilitated by close proximity, prolonged contact, and frequency of contacts. So, the longer the time you spend with an infected person and the larger the gathering, the higher the risk is. (3/n) (https://t.co/h6KQ0pS9aM) pic.twitter.com/BEXhX7jjYP
— Muge Cevik (@mugecevik) January 11, 2021
~ ~ ~
Study: Colleges can prevent 96% of COVID-19 infections with common measures
CLEVELAND–The combined effectiveness of three COVID-prevention strategies on college campuses–mask-wearing, social distancing, and routine testing–are as effective in preventing coronavirus infections as the Pfizer and Moderna vaccines approved by the U.S. Food and Drug Administration (FDA), according to a new study co-authored by a Case Western Reserve University researcher.
The research, published in Annals of Internal Medicine, has immediate significance as college semesters are poised to start again–and as the distribution of approved vaccines lags behind goals.
The study found that a combination of just two common measures–distancing and mandatory masks–prevents 87% of campus COVID-19 infections and costs only $170 per infection prevented.
Adding routine lab-based testing to the mix would prevent 92% to 96% of COVID infections. Still, the cost per infection prevented increases substantially, to $2,000 to $17,000 each, depending on test frequency.
Among the study’s other findings:
- About three of every four students–and nearly one in six faculty–would become infected over the semester in the absence of all mitigation efforts.
- Minimal social distancing policies would only reduce infections by 16% in students.
- While closing the campus and switching to online-only education would reduce infections by 63% among students, it would be less effective than opening the campus and implementing a mask-wearing and social distancing policy, which would reduce infections by 87% among students.
https://www.eurekalert.org/pub_releases/2021-01/cwru-scc011221.php
Tips, general reading for public:
StayAtHome
Wash your hands.
Rinse and repeat.
Politics:
One of the saddest tweets I've ever read. https://t.co/hRwww8gRyY
— Steve Silberman (@stevesilberman) January 12, 2021
~ ~ ~
Israel threatens to bomb #Iran if Biden returns to the nuclear deal. Read that again, it’s not just a threat against Iran but also the incoming US President.
— Assal Rad (@AssalRad) January 14, 2021
If only there was a word for the use of violence & intimidation in pursuit of political aims. https://t.co/BehLXC5Bwh
~ ~ ~
She spent 10 days in jail and had an unreasonably high bail set at $25,000…. pic.twitter.com/GyC3uTTtxL
— Shon (@gayblackvet) January 12, 2021
~ ~ ~
News: A top official at FEMA, which has been assisting in preparations for the Inauguration next week, took personal leave to attend Trump’s “Stop the Steal” rally on Jan. 6. It alarmed some staff, who reported it to the IG and FBI. https://t.co/39eVb5xMWr
— Natasha Bertrand (@NatashaBertrand) January 15, 2021
~ ~ ~
No one is safe from COVID-19 until everyone is safe.
— Raouf Mazou (@RaoufMazou) January 14, 2021
Including refugees in national vaccination plans is key to ensuring we protect as many people as possible and finally end the pandemic.
Thank you to Jordan for paving the way. pic.twitter.com/k8RRXd1fBw
~ ~ ~
Thank goodness there is a new doc by Sam Pollard on FBI surveillance of Dr. King because role of COINTELPRO sure isn't in the textbooks. Check link below to view @MLKFBI and read "Why We Should Teach About the FBI’s War on the Civil Rights Movement" here: https://t.co/z6DmEvQfEv https://t.co/3Tj8qIutrn
— Zinn Ed Project (@ZinnEdProject) January 16, 2021
Feel good du jour:
https://twitter.com/TWaltho/status/1349178094335229962?s=20
~ ~ ~
“In Finland, the # of homeless people has fallen sharply. Those affected receive a small apartment & counselling with no preconditions. 4 out of 5 people affected make their way back into a stable life. And all this is CHEAPER than accepting homelessness.” https://t.co/EH3rer007r
— Brent Toderian (@BrentToderian) January 11, 2021
~ ~ ~
“That was a dagger to the heart,” said David Smith, who was a combat medic in Afghanistan, about his fellow vets who participated in the insurrection.https://t.co/jFQnXu9nig
— Julia Davis (@JuliaDavisNews) January 14, 2021
Comic relief:
How has no one referred to the insurrection as "Guns, Germs, and Steal"????
— Dr. Sherry Zaks (@TheDapperChef) January 13, 2021
~ ~ ~
— opinion defends itself facts speak for themselves (@JonathanBuckn13) January 15, 2021
~ ~ ~
this stray dog gives 'blessings' to the devotees at Shree Siddhivinayak Temple in Siddhatek, India
— Humor And Animals (@humorandanimals) January 15, 2021
(jukin copyright management) pic.twitter.com/UVOrgYdi1K
Perspective/Poem
They didn't want to give immigrants toothpaste nor soap but gave Jake his organic food..
— Sailor Michael⚓✈ (@Megawatts55) January 12, 2021
~ ~ ~
On Tuesday, Jamie Raskin buried his son.
— John Hendrickson (@JohnGHendy) January 8, 2021
On Wednesday, he and his daughter fled the Capitol rampage.
On Thursday, he prepared articles of impeachment against the president.
I called him last night to talk about all of it: https://t.co/Wcm9P81ZLh
Bits of beauty:






